What is heart failure?
Heart failure is the inability of the heart muscle to function normally as a pump, allowing oxygen-enriched blood to circulate throughout the body. Blood flow is insufficient to meet the body’s needs.
SYMPTOMS
Heart failure is a condition that progressively worsens. Its frequency increases with age. At first you may not feel any symptoms, but over time your heart will gradually lose its role as a pump and you will start to feel several, if not all, of the following symptoms:
- Shortness of breath is the first tangible symptom of heart failure: first a difficulty in breathing, felt as a simple respiratory discomfort, then a real shortness of breath on exertion, which can worsen by appearing even when at rest. A sign of major aggravation is the fact of being out of breath when lying down, even more than when sitting.
- Fatigue even during minor exertion.
- Swelling of certain parts of the body (legs, abdomen).
- Significant and rapid weight gain
- Palpitations, heart rhythm and conduction disorders
- Decreased blood pressure
- Confusion and/or memory impairment
CAUSES
There are several possible causes of heart failure.
- The most common cause of heart failure is myocardial infarction.
- This creates irreversible damage to part of the heart muscle, which means that the heart can no longer function normally.
- High blood pressure is also a common cause of heart failure. If not properly controlled, it can strain the heart and lead to heart failure.
- Heart valve disease (valvulopathy)
- Heart infection (myocarditis)
- Congenital heart disease
- Endocarditis, damage to the pericardium (sac surrounding the heart)
DIAGNOSIS
In the presence of certain symptoms (shortness of breath, fatigue, edema …), a check-up is necessary. A medical examination allows the doctor to confirm heart failure, to assess its severity and to look for its cause.
To rule out or confirm the diagnosis, your doctor may prescribe one or more of the following diagnostic examinations:
This is an essential examination in cardiology to test for heart problems. It detects heart rhythm disorders, which can indicate heart failure.
An electrocardiogram is an examination that studies the functioning of the heart by measuring its electrical activity. With each heartbeat, an electrical impulse (or ‘wave’) passes through the heart. This wave causes the heart muscle to contract and expels blood from the heart.
An ECG measures and records the electrical activity of the heart.
Why should I have an ECG?
This procedure can be prescribed in various situations:
- for chest pain or palpitations
- to detect arrhythmia (heart rhythm disorders)
- to detect other heart disorderssuch as coronary heart failure (blockage of the arteries supplying the heart), damaged areas of the heart (due to a lack of blood supply or a recent heart attack), dilation of the heart, etc.
- to monitor the heart’s activity in cases of known heart disease
- on emergency admission for chest pain
- during pre-operative assessment
In all these situations, the ECG results are abnormal. The electrical activity observed is irregular, which makes it possible to detect heart problems.
What happens during the exam and how should I prepare?
- It is a painless examination with no injections into the body
- Between 12 and 15 electrodes are placed on the surface of the skin, on different parts of the body such as the arm, leg and chest. The electrodes are kept in place using small suction cups or adhesive stickers
- Sensors in the electrodes detect the electrical activity of the heart
- You usually need to lie down for an ECG
- An ECG takes between five and ten minutes
- The results are plotted on a roll of paper that comes out of the machine bit by bit.
How should I prepare?
There is no need to fast before an ECG, although it is recommended not to smoke for a while before the procedure begins. You will be asked to remove your jewellery and to wear a hospital gown.
What results can I expect from an ECG?
A normal ECG produces a trace known as ‘sinus rhythm’, with differing electrical periods.
The doctor will interpret the trace to detect any abnormalities, which can involve:
- heart rate (normally between 60 and 100 beats per minute)
- the nature of the rhythm (e.g. absence of one of the normal elements of the curve)
- the amplitude of certain waves
- the length of the interval, among others.
This analysis makes it possible to detect any arrhythmia (irregular heartbeat), to test for heart problems such as a recent or ongoing heart attack, a blockage of the coronary arteries, damaged regions of the heart muscle, dilation of the heart’s volume or inflammation of the membrane that covers it.
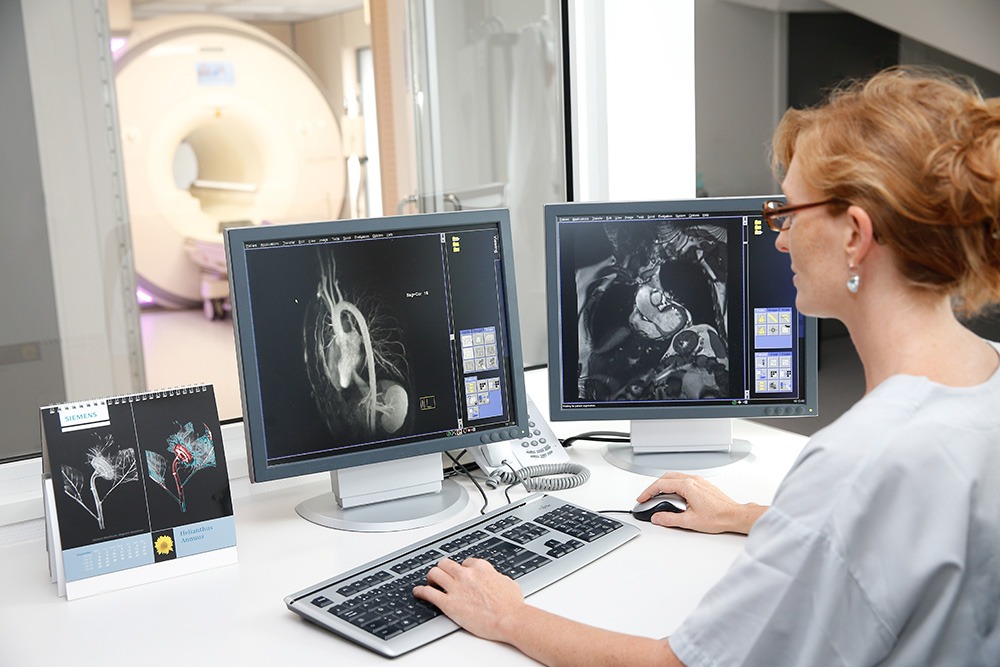
Measures the degree of severity of heart failure, indicates possible causes, and allows complications to be seen.
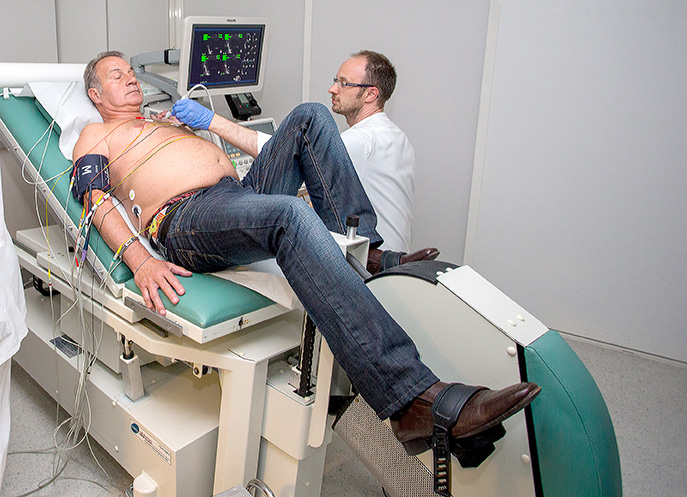
Exercise tolerance (stress) test
Dobutamine stress echocardiogram
This examination is performed by puncturing either the radial artery (at the wrist) or the femoral artery (in the groin fold).
It enables visualisation of the narrowing and occlusion of the arteries.
Combined with fractional flow reserve (FFR) measurement, it can assess whether coronary stenosis leads to a decrease in the blood supply of the heart muscle.
What is coronary angiography for?
Where is coronary angiography performed?
What happens during the exam?
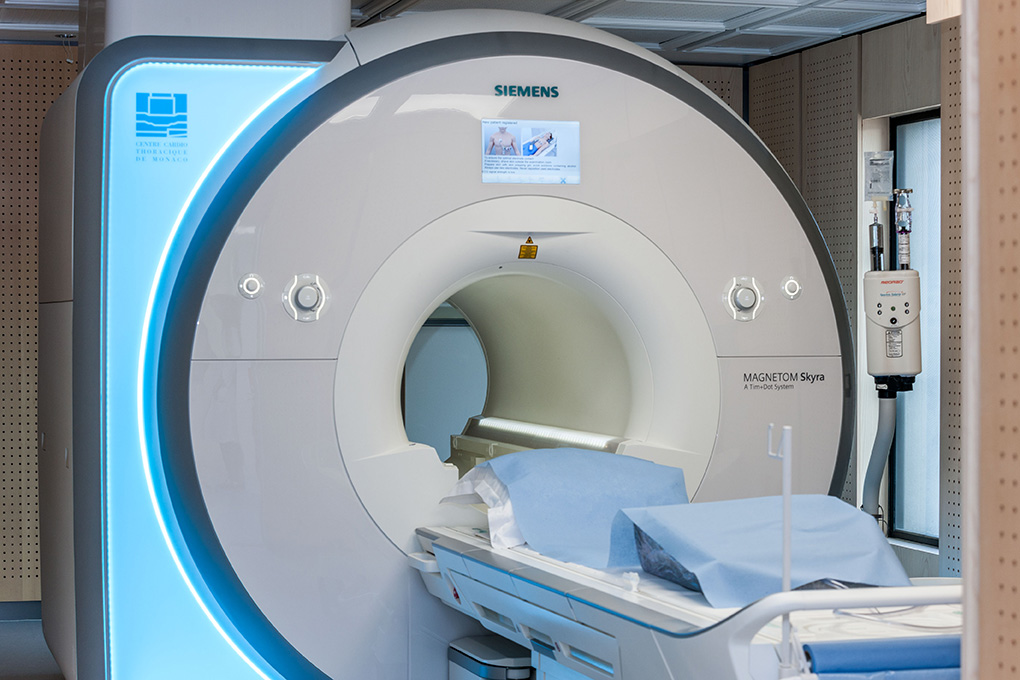
Cardiac MRI allows the morphology and functioning of the heart muscle and valves to be analysed and to detect, for example, a contraction defect in the heart muscle, a narrowed valve, etc…
What is a cardiac MRI?
What happens before, during and after the exam?
Download the explanatory sheet
The particularity of cardiac MRI with Adenosine